
COVID Education
-
Contains 25 Component(s)
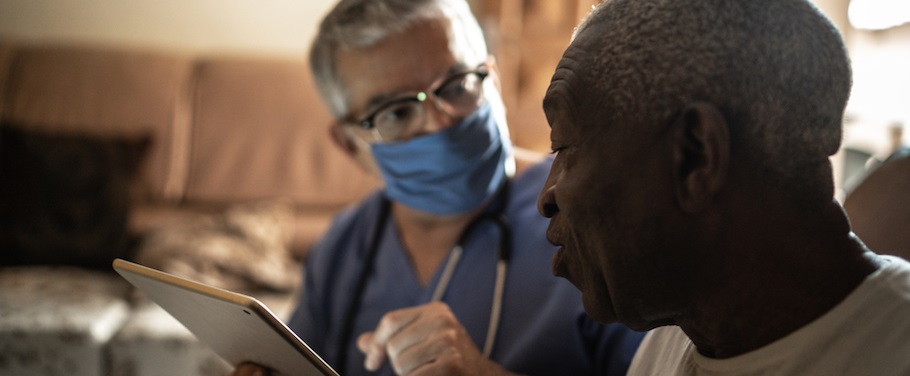
Skilled nursing facilities, assisted living communities, and ID/DD centers are required by OSHA’s Respiratory Protection Standard (29 CFR 1910.134) to establish and maintain a respiratory protection program when employees are exposed to airborne hazards, including infectious agents like COVID-19. Compliance is mandatory to avoid fines and penalties.
AHCA/NCAL, in collaboration with MCA Consulting, LLC, offers a comprehensive Respiratory Protection Plan training and toolkit. This all-in-one resource contains everything needed for full compliance with OSHA’s federal Respiratory Protection Standard, including a customizable template plan, essential forms, training videos, and detailed reference guides.
Stay prepared for airborne disease outbreaks with a comprehensive respiratory protection plan, seamlessly integrated into your infectious disease strategy to safeguard employees and residents. Preparation for any known or potential airborne hazard, as required by CMS and OSHA, ensures readiness for possible future events.
Resources include:
- Comprehensive forms to meet OSHA’s Respiratory Protection Standard and ensure workplace safety
- Step-by-step instructions and video to train appropriate staff on the proper way to perform fit testing
- Customizable templates to tailor the plan to your facility’s unique needs
- Practical guides and tools for seamless implementation and ongoing protection
- Video training for managerial staff and program administrators to maintain a comprehensive plan
- Employee video training to meet OSHA’s annual requirements and promote resident and staff safety
AHCA/NCAL offers a deeply discounted 3-year subscription for this complete all-in-one resource package valued at $4,000+ if purchased through consulting firms.
3-Year Subscription Rates:
AHCA/NCAL Members: $499
Non-members: $699
No CEs awarded upon completion.
How the Subscription Works:
One individual will use their ahcancalED login credentials to subscribe. That individual may then share their ahcancalED login credentials with colleagues to access the subscription for unlimited use of all the resources for three years.
Bulk purchases available. Please contact educate@ahca.org
Specific to this Template Respiratory Plan:
Why am I required to have a Respiratory Protection Program?
OSHA’s Respiratory Protection Standard 29 CFR 1910.134 states that: “in any workplace where respirators are necessary to protect the health of the employee or whenever respirators are required by the employer, the employer shall establish and implement a written respiratory protection program.” While air contaminants can and should be reduced as feasible through engineering controls (i.e. ventilation) and work practice controls (i.e. distancing), the residual risk of exposure can still be high enough to require the use of Personal Protective Equipment (PPE). NIOSH N95 respirators are the last line of defense when it comes to protecting employees from airborne exposure. Thus, proper procedures, training and use are all critical to protection. Additionally, many infectious diseases require the use of airborne precaution protocols. Therefore, employees who encounter patients on airborne isolation precautions are required to wear respiratory protection which is the initial criteria given by OSHA for a respiratory protection program.
How do I customize this Template Plan for my facility?
All Respiratory Programs should include worksite specific procedures. This template plan meets the baseline requirements for a Respiratory Protection Program, as required by OSHA. Organization specific policies and procedures may be included in the “additional notes” sections of the plan. However, any additional procedures added to the template should be carefully followed.
Can I use respirators other than conventional N95s?
There are many types of respirators as well as many levels of filtration. Airborne precautions require an “N95 filtration or greater”. Higher grade filters include but aren’t limited to N99s, N100s, P100s and P99s. N95s are a balance between protection and comfort. They are easiest to breathe through and are typically more readily available in supply chains.
Respirator styles such as elastomeric Full Face and Half Mask Respirators are reusable, but with the use of these types of respirators, comes more stringent maintenance, inspection, cleaning, and storage protocols that are not addressed in this template program. This program is primarily designed for the use of particulate filtering facepiece respirators (N95s) that are used to protect against airborne infectious diseases.
Why does this plan address only infectious diseases? Can I address other hazards?
This plan is tailored to meet the needs of long-term care environments. These environments typically do not deal with hazardous chemical exposures, harmful dusts, or low oxygen levels. Any of these hazards should either be eliminated from the worksite entirely or controlled in a manner to minimize exposure below permissible exposure limits (PELs). See 1910.134(d)(3)(i)(B) (Maximum Use Concentration) and 1910.1000 – (Air contaminants). For more information, see https://www.osha.gov/laws-regs/regulations/standardnumber/1910.
What’s the difference between qualitative and quantitative fit testing methods? Can I use quantitative methods to fit test employees?
Qualitative Fit Testing:
- Method: Relies on the respirator user’s sensory response (taste) to a test agent.
- Process: The user dons a respirator and is exposed to a test substance (e.g., Bitrex (bitter taste), saccharin (sweet taste)).
- Outcome: If the wearer detects the substance, the fit is inadequate; if not detected, the fit is adequate.
This method is typically used for both half-mask respirators and disposable respirators such as N95s.
Quantitative Fit Testing:
- Method: Utilizes instrumentation to numerically measure the fit of a respirator.
- Process: Typically involves a particle counting device or a machine that measures leakage around the mask.
- Outcome: Provides a numerical measurement of the fit factor, which indicates the level of protection provided by the respirator.
This method can be used for both half-face and full-face respirators. There are probe devices that can be inserted into particulate filtering facepieces as well that allow for this method to be used.
Which employees must meet the requirements of the Respiratory Protection Plan (be trained, medically cleared, and fit tested)?
Any employee who is required by their employer to wear a respirator as part of their work duties falls within the scope of the OSHA’s respiratory protection requirements and this respiratory protection plan. All employers are required to assess the workplace for respiratory hazards and provide appropriate respirators for employees when necessary.
Some employees may prefer to wear a respirator even when it is not required. Disposable N95 Respirators can be worn under the Voluntary Use policy. Employees who do not have to wear a respirator as part of their job duties, may still choose to wear a respirator.
Employees are not required to be medically cleared and fit tested WHEN:
- They choose to voluntarily wear a disposable N95 respirator,
- And are outside the known hazardous areas where respiratory protection is required.
What type of circumstances would require program updates and retraining?
The Respiratory Protection Plan should be updated as needed. A few scenarios where this would come into play includes:
- Any change in procedures
- A change in Program Administration
- A new identified hazard in the workplace
- Respirator use issues that are observed in routine audits
- A change in the type of respirators used at a workplace (Introduction of Half Mask or Full-Face Respirators)
- Deficiencies from program audits that show room for improvement
- Regulatory changes
Regular review and updating of the RPP ensure that it remains effective in protecting employees from respiratory hazards and compliant with OSHA regulations.
Respiratory Protection Program:
Do all elements of a respiratory protection program need to be in writing?
Yes, all worksite-specific procedures and elements for required respirator use must be documented in writing. Not all worksites are equal. Some requirements in the OSHA Respiratory Protection Standard may not be applicable to every organization (i.e. an organization that used only disposable respirator models would not have to have procedures for changing out respirator filters).
How often should the written respiratory protection program be updated?
The program should be updated whenever there are changes in the workplace or in respirator use, such as new respirator choices, changes in fit testing, or changes in work operations.
Program Administrator:
How will the Compliance Safety and Health Officer (CSHO) determine if a person is qualified and trained to be a respirator program administrator?
The CSHO will review the written program and interview the program administrator to assess their familiarity with the respirator standard and the use of respirators in the workplace.
Does the standard provide a list of approved training courses for program administrators?
No, OSHA only requires the program administrator to have sufficient training to manage the complexity of the respirator program at the worksite.
Who is qualified to be a Program Administrator?
There is not a discipline qualification requirement for Program Administrator. Infection Preventionist is always a good option, but not required. The responsible person must be able to maintain the components of the program and be able to communicate with OSHA on the program.
Respirators:
What is meant by the conditions of a respirator’s certification?
Respirators are certified by NIOSH as an assembly. Conditions of certification include the limitations of use specified by NIOSH. Parts from other manufacturers or models cannot be substituted.
How many respirator models and sizes are sufficient?
The standard is performance-based; there must be enough models and sizes to ensure all users can achieve an acceptable fit.
Medical Evaluation:
Can a fit test for a respirator be performed before the initial medical evaluation has been completed?
No, the initial medical evaluation must be conducted before fit testing to identify individuals whose health may be harmed by even the limited use of a respirator during fit testing.
Does the medical questionnaire have to be administered by a PLHCP (Physician or other Licensed Healthcare Professional)?
No, the standard does not specify the qualifications of the individual who administers the medical questionnaire, but the employee must be able to discuss the results with the PLHCP.
Are physicians the only medical professionals allowed to perform medical evaluations for respirator use?
No, various healthcare professionals can perform medical evaluations depending on the scope of practice permitted by the state’s licensing, registration, or certification agencies.
Who is an “other Licensed healthcare professional” for purposes of reviewing medical questionnaires?
Under the Respiratory Protection Standard (29 CFR 1910.134), an "other licensed healthcare professional" (OLHCP) is defined as a person whose legally permitted scope of practice (i.e., license, registration, or certification) allows them to independently provide or be delegated the responsibility to review and approve someone for fit testing. Review of the questionnaire does not necessarily require a medical evaluation; therefore, an MD is not always necessary.
An OLHCP can be, but not limited to:
- Physicians
- Registered Nurses (RNs)
- Physician Assistants (PAs)
- Nurse Practitioners (NPs)
Can an employee decline to be medically evaluated for the use of a respirator?
No, an employee cannot refuse the medical evaluation and still use a respirator. The employer must provide a medical evaluation before the employee uses a respirator in the workplace.
What are the recordkeeping requirements for the Medical Questionnaire?
OSHA guidelines regarding the retention of completed Medical Questionnaires can be unclear, particularly when facility staff such as an RN or NP act as the facility’s Licensed Health Care Professional (PLHCP). It's important to note that OSHA’s confidentiality requirements specifically apply to the Medical Questionnaire itself, not the Clearance Form. The Clearance Form, which indicates an employee's medical clearance to use respiratory protection, should be kept in the employee’s training or other records according to your facility’s policies and procedures. This ensures proper documentation while maintaining the confidentiality of the Medical Questionnaire.
What You Can Do with Completed Medical Questionnaires
- If your medical director serves as your PLHCP:
- Request that they retain the completed Medical Questionnaires off-site.
- If you use an outside third-party provider as your PLHCP:
- Ensure that the individual or organization is solely responsible for retaining the completed Medical Questionnaires off-site.
- On-site retention by a staff PLHCP:
- A staff member serving as the facility’s PLHCP may retain the Medical Questionnaires on-site, provided they are the only individual with access to these records and are not serving as an employee’s supervisor.
- Third-party vendors:
- Utilize a third-party vendor or medical professional to retain your Medical Questionnaires securely.
What You Should Never Do with Completed Medical Questionnaires
- Sharing with Management, Supervisors, or Employees:
- Never share completed Medical Questionnaires with management, supervisors, or employees, as these are considered private medical records.
- Inclusion in Personnel or Training Files:
- Never keep completed Medical Questionnaires in an employee’s personnel or training file, or any other file that others can access.
- Access by Non-PLHCP Staff:
- Do not share completed Medical Questionnaires with management, the employee’s supervisor, or any other staff who are not serving as the facility's PLHCP and medical reviewer. (Note: An employee’s supervisor should never serve as the PLHCP responsible for completing or receiving Medical Questionnaires and should not have access to the information contained in these questionnaires.)
- Leaving Documents Unsecured:
- Never leave a completed Medical Questionnaire in a location where others might see it, such as on a desk, in an unlocked file cabinet, in a garbage can, or at the nurse’s station.
Does the employer have to medically reevaluate the employee’s ability to wear a respirator on an annual basis?
No, there is no annual or periodic requirement for medical reevaluation. The standard specifies four conditions that trigger medical reevaluation: when an employee reports signs or symptoms related to the ability to wear a respirator; when the PLHCP, administrator, or supervisor deems it necessary; when information from the respiratory protection program indicates a need for reevaluation; or when a change in workplace conditions substantially increases the physiological burden on the employee.
Do respirators and surgical masks provide the same type and level of protection for the user?
No, respirators and surgical masks serve different purposes and offer varied levels of protection. Surgical masks are primarily used for source control, safeguarding patients from healthcare workers' secretions and large droplet splashes. They are loose-fitting, disposable, and lack a tight seal to the face, thus not effectively filtering airborne particles. Consequently, they do not shield the wearer from inhaling airborne particles transmitted by coughs, sneezes, or certain medical procedures. In contrast, respirators provide a higher level of protection by forming a tight seal to the face and filtering out airborne particles, making them suitable for preventing exposure to airborne transmissible diseases.
Fit Testing:
How many respirators must be available for an employee to choose from when picking out their respirator?
There must be a sufficient variety of respirator models and sizes available so that the user can select one that fits properly and is acceptable for their use.
Can an employee wear a tight-fitting respirator with a beard or other facial hair?
No, employees with facial hair that interferes with the sealing surface of the respirator facepiece are prohibited from wearing tight-fitting respirators when they are required.
Does a “user seal check” qualify as a fit test?
No, a User Seal Check is a procedure performed by the employee each time they put on the respirator to ensure it is properly sealed to their face. It is not a substitute for a fit test, which evaluates the fit of a specific type, model, and size of respirator on an individual.
Is there a certification for a person to obtain before conducting a fit test?
No. The OSHA standard only requires the individual conducting a fit test to be competent in the process.
Training:
Does the standard specify the format or method of training?
The standard is performance-oriented regarding training format. Employers may use any effective training method for their specific worksite as long as it covers the required topics. This could include audiovisual presentations, classroom discussions, informal talks during safety meetings, or a mix of these methods.
Program Evaluation:
How often should the respirator program be re-evaluated?
Employers must review and revise the written program elements specified in paragraph (c)(1) as necessary whenever workplace conditions affecting respirator use change. There is no requirement for an annual review, but rather a review and revisions are needed as workplace conditions change. The frequency of evaluation depends on factors such as program complexity, workplace hazards, types of respirators used, variability of processes, number of respirator users, and worker experience. Employers must ensure continuous, successful implementation of all written program elements through regular review of respirator use in the workplace.
-
Register
- Non-member - $699
- Member - $499
- *Further discounts may apply once you log in.
- More Information
-
Contains 37 Component(s), Includes Credits
Component Credit Type State/Medical Type Available Credits Earned Credits NAB Certificate of Completion: 20240511-22-A94425-DL Medical NAB 24.50 0.00 ANCC Contact Hours Certificate Medical ANCC 24.50 0.00 Welcome!
AHCA/NCAL’s Infection Preventionist Specialized Training (IPCO) is recommended for individuals responsible for infection prevention and control in all long term care settings and is specifically tailored to train Infection Preventionists (IPs) in nursing facilities.
CMS mandates that every nursing facility have a designated and specially trained Infection Preventionist who is running a comprehensive infection prevention and control program. AHCA recommends that nursing facilities train at least two clinical staff members as IPs should one IP leave or be unavailable.
The comprehensive IPCO training covers:
- COVID-19
- Other common pathogens
- Multidrug-resistant organisms
- Antibiotic stewardship
- Water management and more
About the online training:
- Flexible and self-paced (take up to 12 months to complete)
- Online learning 24/7
- 9 course modules
Cost: $450 AHCA/NCAL members |$650 Non-members.
Group purchase with discount structure is available for groups of five or more. There are no refunds and no transfers. Visit the FAQs to know more about the discount offered.
Objectives
Individuals who successfully complete this course will learn how to:
- Demonstrate how to effectively manage an Infection Prevention and Control Program within a nursing or assisted living facility
- Convey to staff effective strategies to prevent infections
- Implement practices and procedures to mitigate infections
- Evaluate practices and policies related to infection prevention
- Provide on-going education to others including staff, residents and families
Individual module objectives are found in the module resource tab within the module presentations and in the User Guide. Participants must complete all training modules and successfully pass module quizzes and final test with a grade of 80 or above to receive a certificate of completion from AHCA that is valid for three years.
Accredited Continuing Education
In support of improving patient care, this activity has been planned and implemented by University of Nebraska Medical Center and American Health Care Association. University of Nebraska Medical Center is jointly accredited by the Accreditation Council for Continuing Medical Education (ACCME), the Accreditation Council for Pharmacy Education (ACPE), and the American Nurses Credentialing Center (ANCC), to provide continuing education for the healthcare team.
NURSES/NURSE PRACTITIONERS
The University of Nebraska Medical Center designates this activity for 24.5 ANCC contact hours. Nurses should only claim credit for the actual time spent participating in the activity.
Certificates
Three certificates will be awarded upon successful completion of the program:
- UNMC CON CiPDI will provide a certificate awarding 24.5 contact hours.
- AHCA will provide a Specialized Training Completion certificate, valid for 3 years.
- 24.5 continuing education hours (CEs) from the National Association of Long Term Care Administrator Boards (NAB)
Certificates Renewal - specialized training completion certificates are valid for 3 years. Click here for information about renewing your AHCA IPCO Certificate.
If you are not sure of your member status, please email educate@ahca.org before making payment.
© 2025 American Health Care Association. All rights reserved. All Infection Preventionist Specialized Training (IPCO) materials subject to this copyright may be photocopied or distributed for the purpose of nonprofit or educational advancement. The use, photocopying, and distribution for commercial purposes of any of these materials is expressly prohibited without the prior written permission of American Health Care Association.
Holly Harmon, RN, MBA, LNHA, FACHCA
Senior VP, Quality, Regulatory & Clinical Services
American Health Care Association
Holly Harmon, RN, MBA, LNHA, FACHCA brings both passion anda wealth of practical, real-world, clinical and operational experience to herrole as Senior Director of Clinical Services at AHCA. Her extensive service ina wide array of settings including post-acute care, long term care, residentialcare, assisted living, independent living, a psychiatric hospital andoccupational health have provided her with insights, knowledge, skills andinnovative ideas which she exuberantly shares with others.
In addition to her vast clinical experience, Ms. Harmon hasput her dynamic energy into leading the statewide Maine Culture ChangeCoalition/LANE as President, the Maine Partnership to Improve Dementia Care inNursing Homes as Co-Chair, Vice-President of American College of Health CareAdministrators, Maine Chapter and the Maine LANE Co-Convener for the nationalAdvancing Excellence in America’s Nursing Homes Campaign. She also served asthe Director of Quality Improvement & Regulatory Affairs at the MaineHealth Care Association.
She puts her boundless energy and warm and energeticpersonality into training, education and presenting both, nationally andlocally. She has made simplifying the complex world of long term and post-acutecare policy and practice an art.
David Gifford, MD, MPH
Chief Medical Officer , AHCA
Chief Medical Officer, AHCA David Gifford, MD, MPH, is a geriatrician and former medical director of several nursing homes in Rhode Island. He currently serves as the Chief Medical Officer at the American Health Care Association. He helped create the Quality Department at AHCA which assists providers in their quality improvement efforts and works with administration officials on regulations and policies impacting the profession.
Dr. Gifford also serves on the Board of the Advancing Excellence in America’s Nursing Homes campaign and the Baldrige Foundation Board. He is a former Director of the Rhode Island State Department of Health, where he received the National Governor’s award for Distinguished Service Award for State Officials. Prior to that he served as Chief Medical Officer for Quality Partners of Rhode Island where he directed CMS’ national nursing home-based quality improvement effort. He also holds a faculty appointment at Brown University Medical School and School of Public Health. He received his medical degree from Case Western Reserve University and conducted his geriatric fellowship at UCLA where he also earned his Master’s in Public Health while a Robert Wood Johnson Clinical Scholar.
Amy Miller, RN, BSN, RAC-CT, CPC
Director, Clinical & Regulatory Services
American Health Care Association
Amy Miller is currently the Director of Clinical and Regulatory Services with the American Health Care Association. She is a registered nurse with over 25 years of experience in skilled nursing and long-term care. She has her Bachelor of Science Degree in Nursing from Misericordia University in Pennsylvania, is a certified professional coder with the AAPC, and is also a certified resident assessment coordinator.
Marguerite McLaughlin, BS, MA
Director of Education and Transformation, Healthcentric Advisors
MARGUERITE M. McLaughlin is the Director of Education and Transformation, Healthcentric Advisors . She has worked in the nation’s capital as Senior Director of Quality Improvement at AHCA. She pursues her passion for improving the lives of residents living in long term care centers by developing educational resources, tools and products for staff, and consulting with staff to improve quality within nursing centers. Ms. McLaughlin is an enthusiastic educator and trainer working both locally and nationally to support change in healthcare. Her 30+ years of experience – at Saint Elizabeth Home, the Alzheimer’s Association and the Healthcentric Advisors (the state’s Quality Improvement Organization) have provided her with unique insights and “boots on the ground” experience in helping organizations improve care and service to their residents. She has served as liaison to the Industry Partnership for Healthcare under the Governor’s Workforce Board-Rhode Island. In this role she provided solutions to bridge the skills gaps within the healthcare industry. She was Co-Chair of SAGE-RI for six years. She earned a Master’s degree in Holistic Counseling at Salve Regina and applies this knowledge to individualized care and organizational culture.
Janet Snipes, NHA
Janet Snipes NHA is currently retired. She served on the Colorado Health Care Association Board of Directors for over 20 years and was the Chairman of the Board from 2004-2014. She served as Chair of the American Health Care Association (AHCA) Quality Improvement Committee from 2010 to 2014.
Stefan Gravenstein, MD, MPH
Director, Geriatrics and Palliative Medicine, Professor of Medicine, Alpert Medical School of Brown University
Warren Alpert Medical School of Brown University
A geriatrician, former John Franklin Chair of Geriatrics and Director of the Glennan Center for Geriatrics and Gerontology at Eastern Virginia Medical School (1996-2007), and Director of Center for Geriatrics and Palliative Care at University Hospitals in Cleveland (2014-2017), Stefan Gravenstein is now the David S. Greer Professor of Geriatrics and Professor in the departments of Medicine and Health Services Policy and Practice at Brown's schools of medicine and public health. He serves as the Director, Division of Geriatrics and Palliative Medicine at the Alpert Medical School of Brown University and Associate Director of the Center on Innovation in Long-Term Services and Supports at the Providence Veterans Administration Medical Center. Dr. Gravenstein has a long-standing interest in immunity, inflammation, cardiovascular outcomes and aging especially in the context of vaccines and the long-term care setting, and the topic of the majority of his publications. He also has a specific interest in quality improvement in health care, the culture of care, antimicrobial stewardship, and how to improve care transitions. Beginning n 2020, he became active in several projects related to COVID in long-term care. He was Clinical Director at Healthcentric Advisors, Medicare's Quality Improvement Organization for New England from 2007 to 2019. Elie Saade, MD, MPH
System Director, Medical Quality and Infection Control, University Hospitals, Cleveland, Ohio
Dr. Elie Saade is System Director, Medical Quality and Infection Control, University Hospitals, Cleveland, Ohio. He specializes in infectious diseases.
Janet Robinson, RN, MEd, CIC
Retired
Ms. Robinson is currently retired. She was board certified in infection control with more than twenty-five years of consulting experience in long-term care facilities. She was an accomplished public speaker and educator in the area of long-term care infection control. In collaboration with the Rhode Island Department of Health as well as the American Health Care Association, she contributed to the development of guidelines and training materials.
Linda Behan, BSN, RN, CIC
Consultant, Long Term Care Infection Prevention, LLC
Linda Behan BSN, RN, CIC is the Consultant for Long Term Care Infection Prevention, LLC . Linda has been certified in infection prevention and control for over 10 years. She leads a team of Infection Preventionists in developing policies and procedures as well as developing and delivering education across the company. Linda serves on the APIC Professional Development Committee and frequently presents at healthcare and professional organization conferences.
Gail Polanski, RN, BSN
Clinical Consultant, Tara Cares, LLC
Gail Polanski RN, BSN serves as Clinical Consultant, Tara Cares, LLC. Gail has more than 30 years of experience in senior management positions. Her expertise includes the delivery of rehabilitation services, denials management, compliance, and case mix management. She is knowledgeable of Medicare regulations and managed care contractual requirements.
Prior to joining Tara Therapy, Gail was an independent consultant and entrepreneur. As owner of MG Healthcare Solutions, she provided consulting services to clients across the country on the changing Medicare payment program and SNF PPS regulations. Gail has presented at national conventions and is currently an active member of the AHCA Clinical Practice Committee and serves as the co-chair for the MDS/IMPACT subcommittee.
Stacey Merritt Hord, LNHA, MCD, CCC-SLP
Chief Business Development Officer, Associated Care Ventures
Stacey Merritt Hord is the 2016/2017 Chair of the AHCA/NCAL Quality Improvement Committee and Vice President of Quality for Golden Living, the 3rd largest long term care provider in the country. Stacey is a health care executive with expertise in educating, deploying and sustaining Baldrige as a Business Model in post acute care and other sectors. Facilities under her operational oversight as an LNHA received AHCA Bronze and Silver recognition along with Alabama Level 1 Commitment to Excellence, Level 2 Progress Toward Excellence, and Level 3 Alabama Excellence recognition. Her faculty experience includes the AHCA/NCAL national convention, Alabama Quality Award Conference, AHCA Quality Symposium/Summit, Georgia Health Care Association Convention, and other venues. Stacey served on the panel of experts for the AL Quality Award Conference from 2004 - 2008 and has served as an AHCA Quality Award Examiner in multiple roles (Bronze, Silver, Silver Team Leader, Master Examiner) since 2002. She served as a member of the AHCA Quality Improvement Committee (QIC) and AHCA QAPI subcommittee from 2012- 2015. In addition, Stacey served as Chair of the 2015 QAPI Tools and Resources WorkGroup for the Quality Improvement Committee.

Frequently Asked Questions
What is the AHCA Infection Preventionist Specialized Training (IPCO)?
It is a specialized training for healthcare professionals who desire to serve as Infection Preventionists (IPs) as established in the CMS Reform of Requirements of Participation for Long Term Care Facilities (required by November 2019). Through this program, individuals will be specially trained to effectively implement and manage an Infection Prevention and Control Program in a nursing center.
Do you have to be an AHCA member to register for IPCO?
No. Both AHCA members and nonmembers are eligible to participate in the IPCO course.
How much does it cost to take the IPCO training?
Registration fee: $450 members, $650 nonmembers. Payment and registration is completed by individual participant in the IPCO product in ahcancalED.
How can an individual register and pay for IPCO?
The individual who wants to take the IPCO course must login to ahcancalED and register for the course under their individual login. Payment will be made in ahcancalED upon registration via credit card or E-check. Please be sure to have your credit card or banking information ready at checkout. Paying by credit card or E-check will grant automatic access to the course. Registrations for IPCO cannot be done by another person or under another person’s ahcancalED login.
-- for a better web experience, please use Google Chrome Internet Browser and NOT Internet Explorer.
How can an organization group register and pay for IPCO?
Group purchase is available for groups of 5 or more. AHCA offers the following discount structure for groups: 5-49 registrations will receive $25 off each registration. 50 or more registrations will receive $75 off each registration.
After full payment is made for group purchase of IPCO, the designated individuals who the IPCO registration payment was made for, will be provided with a unique group code for their group which will translate to $0 due upon registration (because full payment has already been received). One code will be provided for each group with a max allowance of times that the code can be used based on the group’s payment.
Each individual will need to login to the AHCA website to access ahcancalED and then complete their own registration using the group code.
Can I get a refund on the IPCO product if I no longer want to take the course?
No refunds are issued for IPCO.
Can my IPCO registration be transferred to a colleague?
IPCO registrations cannot be transferred. The individual that registers for the course is the only one that has access to it.
Who is eligible to take this training?
Anyone can take this training. The AHCA Infection Preventionist Specialized Training does not require a particular healthcare license.
AHCA/NCAL recommends that administrators also consider taking the course to gain a deeper understanding of infection prevention and control in the overall operation of the building. Just a reminder that administrators should not serve as designated Infection Preventionists unless they have separate formal advanced clinical training and/or licensing such as a nursing license.
Please note, there are specific requirements for the individual(s) who will serve as Infection Preventionist(s). CMS requirements for a designated Infection Preventionist state:
483.80 (b) Infection preventionist. The facility must designate one or more individual(s) as the infection preventionist(s) (IPs) who are responsible for the facility’s IPCP. The IP must:
(1) Have primary professional training in nursing, medical technology, microbiology, epidemiology, or other related field;
(2) Be qualified by education, training, experience or certification;
(3) Work at least part-time at the facility; and
(4) Have completed specialized training in infection prevention and control.
What are the requirements to successfully complete IPCO?
Participate in each module and successfully complete quizzes throughout the course and final test (achieve at least 80% correct each time)
Modules 1-7 will have quizzes with 5 questions (4 of 5 questions must be accurately completed) except for module 3 which will have 10 questions (8 of 10 questions must be accurately completed).
The final test after Module 9 will have 20 questions (16 of 20 questions must be accurately completed)
Each module quiz may be attempted three times before the participant is required to repeat the module and then reattempt answering questions.
Complete course evaluation after each module and at the end of the course.
Course completion must occur within 12 months of the date the registrant starts the first required component of the program; which is the copyright agreement.(not registration date)
How long does it take on average to complete the IPCO course?
The learning time of all modules, review of additional resources, time to complete the modules and final course evaluations and quizzes/final test accounts for 24 hours and 30 minutes.
Participants are encouraged to spread out the course over time in an organized manner – such as scheduling module reviews on various dates/times when they can focus their attention to it. The course could be completed within a week or over several months based on how the individual would like to approach the program.
Are Contact Hours awarded for IPCO?
Yes, 24.5 ANCC contact hours and 24.5 continuing education hours (CEs) from the National Association of Long Term Care Administrator Boards (NAB) are available for completion of this program.
In support of improving patient care, this activity has been planned and implemented by University of Nebraska Medical Center and American Health Care Association. University of Nebraska Medical Center is jointly accredited by the Accreditation Council for Continuing Medical Education (ACCME), the Accreditation Council for Pharmacy Education (ACPE), and the American Nurses Credentialing Center (ANCC), to provide continuing education for the healthcare team.
What does a participant get when they complete the IPCO course?
Participants receive three certificates at the completion of IPCO:
- UNMC CON CiPDI will provide a certificate awarding 24.5 contact hours to participants who successfully achieve the completion requirements.
- 24.5 continuing education hours (CEs) from the National Association of Long Term Care Administrator Boards (NAB)
- Specialized Training Completion certificate from AHCA, valid for 3 years.
How long do the certificates last?
The CE certificates do not expire. The Specialized Training Completion certificate expires after 3 years from issue date.
How can someone renew their IPCO certificate?
Renewal may occur by the options below:
Option 1: Registering for a competency exam requiring a grade of 80% or above to successfully receive certificate of renewal. This option is only available to individuals who have previously successfully completed the full IPCO course and are seeking renewal.
Option 2: Registering for the IPCO course and completing the course requirements as outlined above.
Is IPCO a certification?
No, IPCO is a specialized training program with a certificate upon successful completion. While it is not a certification, IPCO does meet both the content and intensity/duration of CMS requirements to serve as an Infection Preventionist.
Does IPCO meet CMS requirements?
Yes, IPCO meets the expectations CMS has outlined on the required components of the specialized training.
CMS is not endorsing any particular training, rather CMS is focused on the content and intensity/duration of what will meet the specialized training requirement. Based on information AHCA received from CMS, the IPCO training meets both the content and intensity/duration of CMS requirements.
Can I print the presentation slides and how can I access the resources within the module?
Each module contains a resource guide which includes a copy of the presentation and any necessary supporting documents discussed within the module. This resource guide can be found at the top right corner within each module.
I am having technical difficulties with IPCO, can you help?
Please email us at educate@ahca.org.
"What a great program! I was able to complete at my own pace and learned a lot." - Connie Francioli, RN,WCC, Director of Nursing, Odd Fellow & Rebekah Rehabilitation RHCC Inc.
"The AHCA IPCO program gave me the tools I needed to be effective in my role as the Infection Preventionist and to initiate an antibiotic stewardship program. The modules and website were easy to navigate and very convenient for my schedule. Thanks a bunch!"- Adriana Casale, BSN, RN, Assistant Director of Nursing Services, Roberts Health Centre
"I thoroughly enjoyed the course. I am a new to the Infection Prevention world and this engaging and interactive course provided an excellent foundation for me. I hope to use this as a stepping stone to advance the Infection Prevention culture within my facility and my community." - Daniel Mazzone, Associate Director of Nursing and Infection Preventionist at the Acadia Center for Nursing
"The IPCO training was intense but I gained the confidence to implement key initiatives in our facility, including antibiotic stewardship. I have a lot to learn but I know I can go back to the course and get the information I need with any situation that I am confronted with." - Karla Ruther, Clarence Senior Living Director of Nursing
"I really enjoyed the IPCO program. It is full of knowledge and information for any infection control program. I would like to see more infection control class with updates on organisms and new ROPs." - Helen Durden, RN, Education Coordinator, Eagle Health and Rehabilitation
"This course was a good blend of review, new information and practical tools for program improvement in both skilled and long term care settings. I would recommend for any nurse interested in Infection control and prevention." - Becci St Laurent | Senior Director of Education, Palm Healthcare Management, llc
"I am recommending it to our Corporate Team members here at Laurel Health Care. I know some Associate Team members at Ciena Heath Care have taken this training program, as well, and were very satisfied. It really enhances and clarifies so much Infection Control information. I feel much more confident with being and Infection Control practitioner." - Marlissa Corby, Corporate Compliance Officer, Laurel Health Care Company
How can an organization group register and pay for IPCO?
One user can purchase multiple registrations for other users by adding them to their cart during the checkout process; using the button displayed in image below. (This can only be done if all individuals have an ahcancalED account.) The price of the training will be based on each registrant’s member type (member or non-member).
*payment tip: please be sure when you are paying with a credit card the bill-to and shipping address are the same*
Group purchase is available for groups of 25 or more. If you are interested in group purchasing, please email educate@ahca.org
After full payment is made for group purchase, the designated individuals who the course registration payment was made for, will be provided with a unique group code for their group which will translate to $0 due upon registration (because full payment has already been received). One code will be provided for each group with a max allowance of times that the code can be used based on the group’s payment.
Each individual will need to login to the AHCA website to access ahcancalED and then complete their own registration using the group code.
PLEASE NOTE THAT WE ONLY ACCEPT PAYMENT IN THE FORM OF A CHECK FOR GROUP PURCHASES.
The NIPF is a national forum for any infection preventionist (IP) or infection prevention champions in long-term care (LTC) to share lessons learned and resources and get answers to questions.
This national forum will also provide a mechanism to rapidly disseminate federal updates and resources about infections in LTC as they become available from Centers for Disease Control and Prevention (CDC), Centers for Medicare and Medicaid Services (CMS), or Occupational Safety and Health Administration (OHSA). The American Health Care Association (AHCA) partnered with the Association for Professionals in Infection Control and Epidemiology (APIC) with funding from CDC Project First Line to set up the NIPF, which is open to all LTC professionals focusing on infection prevention regardless of their membership in AHCA or APIC.
The goal of NIPF is to foster collaboration and sharing of experiences between IPs in LTC. In addition, APIC and CDC subject matter experts will be available to address questions the group are unable to answer. There are designated threads for Hot Topics, Ask the CDC Expert, and test your clinical skills using Clinical Based Scenarios. The NIPF uses the “Connect Communities” platform to organize email discussions by threads and allows for sharing and posting of resources and tools in an organized library and ability to look up other IPs participating in the forum. You can receive email updates for threads in real-time or daily summaries.
To enroll in this national forum, all you need to do is fill out our form here https://www.ahcancal.org/Quality/Pages/NIPF and our team will process your application. If you have questions, please feel free to contact us at LTC-NIPFhelp@ahca.org.
-
Register
- Non-member - $650
- Member - $450
- *Further discounts may apply once you log in.
- More Information
-
Contains 37 Component(s), Includes Credits
Component Credit Type State/Medical Type Available Credits Earned Credits NAB Certificate of Completion: 20250505-28.75-A103131-DL Medical NAB 28.75 0.00 ANCC Contact Hours Certificate Medical ANCC 25.50 0.00 
Now more than ever, an Infection Prevention Control Officer is critical to have in your building/organization. AHCA/NCAL Infection Preventionist Specialized Training (IPCO) for Assisted Living, is a specialized course of study for healthcare professionals who desire to serve as Infection Preventionists (IPs) in a Long Term Care setting, which is a requirement by CMS for skilled nursing centers. With this version for assisted living, we’ve added information on how these concepts can also be applied to the assisted living setting but still also contains information necessary to be recognized by CMS as having received additional training in infection control. Through this program, individuals will be specially trained to effectively implement and manage an Infection Prevention and Control Program in either assisted living or skilled nursing centers.
The American Health Care Association/National Center for Assisted Living is happy to announce the launch of the assisted living version of the Infection Prevention Control Officer (IPCO) training. This updated version incorporates information from the COVID-19 pandemic, the most recent regulatory requirements as well as sections on Candida auris, Multi-Drug Resistant Organisms (MDROs), and Enhanced Barrier Precautions (EBP). Additionally, there is an entire section on how to get an effective water management program running in your center.
The Assisted Living IPCO Training includes:
- Added:
- Multi-drug Resistant Organisms (MDROs) and Enhanced Barrier Precautions (EBP)
- Candida auris
- Water management program
- COVID-19
- 25.5 ANCC Contact Hours and 28.75 hours of continuing education credit for Nursing Home Administration and Residential Care/ Assisted Living Administration
- Updated regulatory requirements for Skilled Nursing Facilities that make this version eligible to meet the requirements for both SNF and assisted living facilities
The training is an online, self-study program on ahcancalED. The training includes online lectures, case studies, and interactive components taught by an array of experts from around the country.
Objectives
Students who complete this course successfully will be able to:
- Demonstrate how to effectively manage an Infection Prevention and Control Program within my healthcare setting
- Convey to staff effective strategies to prevent infections
- Implement practices and procedures to mitigate infections
- Evaluate practices and policies related to infection prevention
- Provide ongoing education to others including staff, residents, and families
Cost: $450 AHCA/NCAL members | $650 Non-members.
Group purchase with discount structure is available for groups of five or more. There are no refunds and no transfers. Visit the FAQs to know more about the discount offered.
Accredited Continuing Education
In support of improving patient care, this activity has been planned and implemented by University of Nebraska Medical Center and American Health Care Association. University of Nebraska Medical Center is jointly accredited by the Accreditation Council for Continuing Medical Education (ACCME), the Accreditation Council for Pharmacy Education (ACPE), and the American Nurses Credentialing Center (ANCC), to provide continuing education for the healthcare team.
NURSES/NURSE PRACTITIONERS
The University of Nebraska Medical Center designates this activity for 25.5 ANCC contact hours. Nurses should only claim credit for the actual time spent participating in the activity.
Certificates
Three certificates will be awarded upon successful completion of the program:
- UNMC CON CiPDI will provide a certificate awarding 25.5 contact hours.
- AHCA/NCAL will provide a Specialized Training Completion certificate, valid for 3 years.
- 28.75 continuing education hours (CEs) from the National Association of Long Term Care Administrator Boards (NAB)
Certificates Renewal - specialized training completion certificates are valid for 3 years. Click here for information about renewing your AHCA IPCO Certificate.
If you are not sure of your member status, please email educate@ahca.org before making payment.
© 2024 American Health Care Association. All rights reserved. All Infection Preventionist Specialized Training (IPCO) for Assisted Living materials subject to this copyright may be photocopied or distributed for the purpose of nonprofit or educational advancement. The use, photocopying, and distribution for commercial purposes of any of these materials is expressly prohibited without the prior written permission of American Health Care Association.
Holly Harmon, RN, MBA, LNHA, FACHCA
Senior VP, Quality, Regulatory & Clinical Services
American Health Care Association
Holly Harmon, RN, MBA, LNHA, FACHCA brings both passion anda wealth of practical, real-world, clinical and operational experience to herrole as Senior Director of Clinical Services at AHCA. Her extensive service ina wide array of settings including post-acute care, long term care, residentialcare, assisted living, independent living, a psychiatric hospital andoccupational health have provided her with insights, knowledge, skills andinnovative ideas which she exuberantly shares with others.
In addition to her vast clinical experience, Ms. Harmon hasput her dynamic energy into leading the statewide Maine Culture ChangeCoalition/LANE as President, the Maine Partnership to Improve Dementia Care inNursing Homes as Co-Chair, Vice-President of American College of Health CareAdministrators, Maine Chapter and the Maine LANE Co-Convener for the nationalAdvancing Excellence in America’s Nursing Homes Campaign. She also served asthe Director of Quality Improvement & Regulatory Affairs at the MaineHealth Care Association.
She puts her boundless energy and warm and energeticpersonality into training, education and presenting both, nationally andlocally. She has made simplifying the complex world of long term and post-acutecare policy and practice an art.
David Gifford, MD, MPH
Chief Medical Officer , AHCA
Chief Medical Officer, AHCA David Gifford, MD, MPH, is a geriatrician and former medical director of several nursing homes in Rhode Island. He currently serves as the Chief Medical Officer at the American Health Care Association. He helped create the Quality Department at AHCA which assists providers in their quality improvement efforts and works with administration officials on regulations and policies impacting the profession.
Dr. Gifford also serves on the Board of the Advancing Excellence in America’s Nursing Homes campaign and the Baldrige Foundation Board. He is a former Director of the Rhode Island State Department of Health, where he received the National Governor’s award for Distinguished Service Award for State Officials. Prior to that he served as Chief Medical Officer for Quality Partners of Rhode Island where he directed CMS’ national nursing home-based quality improvement effort. He also holds a faculty appointment at Brown University Medical School and School of Public Health. He received his medical degree from Case Western Reserve University and conducted his geriatric fellowship at UCLA where he also earned his Master’s in Public Health while a Robert Wood Johnson Clinical Scholar.
Marguerite McLaughlin, BS, MA
Director of Education and Transformation, Healthcentric Advisors
MARGUERITE M. McLaughlin is the Director of Education and Transformation, Healthcentric Advisors . She has worked in the nation’s capital as Senior Director of Quality Improvement at AHCA. She pursues her passion for improving the lives of residents living in long term care centers by developing educational resources, tools and products for staff, and consulting with staff to improve quality within nursing centers. Ms. McLaughlin is an enthusiastic educator and trainer working both locally and nationally to support change in healthcare. Her 30+ years of experience – at Saint Elizabeth Home, the Alzheimer’s Association and the Healthcentric Advisors (the state’s Quality Improvement Organization) have provided her with unique insights and “boots on the ground” experience in helping organizations improve care and service to their residents. She has served as liaison to the Industry Partnership for Healthcare under the Governor’s Workforce Board-Rhode Island. In this role she provided solutions to bridge the skills gaps within the healthcare industry. She was Co-Chair of SAGE-RI for six years. She earned a Master’s degree in Holistic Counseling at Salve Regina and applies this knowledge to individualized care and organizational culture.
Janet Snipes, NHA
Janet Snipes NHA is currently retired. She served on the Colorado Health Care Association Board of Directors for over 20 years and was the Chairman of the Board from 2004-2014. She served as Chair of the American Health Care Association (AHCA) Quality Improvement Committee from 2010 to 2014.
Stefan Gravenstein, MD, MPH
Director, Geriatrics and Palliative Medicine, Professor of Medicine, Alpert Medical School of Brown University
Warren Alpert Medical School of Brown University
A geriatrician, former John Franklin Chair of Geriatrics and Director of the Glennan Center for Geriatrics and Gerontology at Eastern Virginia Medical School (1996-2007), and Director of Center for Geriatrics and Palliative Care at University Hospitals in Cleveland (2014-2017), Stefan Gravenstein is now the David S. Greer Professor of Geriatrics and Professor in the departments of Medicine and Health Services Policy and Practice at Brown's schools of medicine and public health. He serves as the Director, Division of Geriatrics and Palliative Medicine at the Alpert Medical School of Brown University and Associate Director of the Center on Innovation in Long-Term Services and Supports at the Providence Veterans Administration Medical Center. Dr. Gravenstein has a long-standing interest in immunity, inflammation, cardiovascular outcomes and aging especially in the context of vaccines and the long-term care setting, and the topic of the majority of his publications. He also has a specific interest in quality improvement in health care, the culture of care, antimicrobial stewardship, and how to improve care transitions. Beginning n 2020, he became active in several projects related to COVID in long-term care. He was Clinical Director at Healthcentric Advisors, Medicare's Quality Improvement Organization for New England from 2007 to 2019. Elie Saade, MD, MPH
System Director, Medical Quality and Infection Control, University Hospitals, Cleveland, Ohio
Dr. Elie Saade is System Director, Medical Quality and Infection Control, University Hospitals, Cleveland, Ohio. He specializes in infectious diseases.
Linda Behan, BSN, RN, CIC
Consultant, Long Term Care Infection Prevention, LLC
Linda Behan BSN, RN, CIC is the Consultant for Long Term Care Infection Prevention, LLC . Linda has been certified in infection prevention and control for over 10 years. She leads a team of Infection Preventionists in developing policies and procedures as well as developing and delivering education across the company. Linda serves on the APIC Professional Development Committee and frequently presents at healthcare and professional organization conferences.
Gail Polanski, RN, BSN
Clinical Consultant, Tara Cares, LLC
Gail Polanski RN, BSN serves as Clinical Consultant, Tara Cares, LLC. Gail has more than 30 years of experience in senior management positions. Her expertise includes the delivery of rehabilitation services, denials management, compliance, and case mix management. She is knowledgeable of Medicare regulations and managed care contractual requirements.
Prior to joining Tara Therapy, Gail was an independent consultant and entrepreneur. As owner of MG Healthcare Solutions, she provided consulting services to clients across the country on the changing Medicare payment program and SNF PPS regulations. Gail has presented at national conventions and is currently an active member of the AHCA Clinical Practice Committee and serves as the co-chair for the MDS/IMPACT subcommittee.
Stacey Merritt Hord, LNHA, MCD, CCC-SLP
Chief Business Development Officer, Associated Care Ventures
Stacey Merritt Hord is the 2016/2017 Chair of the AHCA/NCAL Quality Improvement Committee and Vice President of Quality for Golden Living, the 3rd largest long term care provider in the country. Stacey is a health care executive with expertise in educating, deploying and sustaining Baldrige as a Business Model in post acute care and other sectors. Facilities under her operational oversight as an LNHA received AHCA Bronze and Silver recognition along with Alabama Level 1 Commitment to Excellence, Level 2 Progress Toward Excellence, and Level 3 Alabama Excellence recognition. Her faculty experience includes the AHCA/NCAL national convention, Alabama Quality Award Conference, AHCA Quality Symposium/Summit, Georgia Health Care Association Convention, and other venues. Stacey served on the panel of experts for the AL Quality Award Conference from 2004 - 2008 and has served as an AHCA Quality Award Examiner in multiple roles (Bronze, Silver, Silver Team Leader, Master Examiner) since 2002. She served as a member of the AHCA Quality Improvement Committee (QIC) and AHCA QAPI subcommittee from 2012- 2015. In addition, Stacey served as Chair of the 2015 QAPI Tools and Resources WorkGroup for the Quality Improvement Committee.
Pamela Truscott, DNP/HSL, MSN/Ed, RN, DNS-CT, QCP, RAC-CT, CDP
Director of Quality Improvement
NCAL
Pamela Truscott, DNP/HSL, MSN/Ed, RN, DNS-CT, QCP is the Director of Quality Improvement with the National Center for Assisted Living (NCAL). She joined the AHCA/NCAL family in June 2019 and has been actively involved with a variety of education, tools and resources such as: trauma-informed care, behavioral health, functional outcomes improvement, and infection prevention and control. Prior to joining AHCA, Pam worked for the Nebraska Health Care Association (NHCA) as the Vice President of Professional Development for seven years and is a Nebraska Assisted LIving Administrator. Before joining the NHCA team, she worked in a rural nursing home with attached assisted living community for 15 years in a variety of roles, including: charge nurse, wound nurse, medication aide, and direct care staff member. She is an active member in the American Nurses Association as well as the American Association of Post-Acute Care Nurses. She received a Doctor of Nursing Practice with specialy focus in Healthcare Systems Leadership and Master of Science in Nursing with focus in nursing education degree from Chamberlain College of Nursing. Pam has over 20 years of long-term care experience and shares a passion for growing education and cultivating new leaders in long-term care.

Frequently Asked Questions
What is the AHCA Infection Preventionist Specialized Training (IPCO)?
It is a specialized training for healthcare professionals who desire to serve as Infection Preventionists (IPs) in either Assisted Living or Skilled Nursing Centers. as established in the CMS Reform of Requirements of Participation for Long Term Care Facilities (required by November 2019). Through this program, individuals will be specially trained to effectively implement and manage an Infection Prevention and Control Program in both a skilled nursing center and assisted living and will receive a certificate that is recognized as completing additional training in infection control to meet CMS requirements to serve as an IP in Skilled Nursing Centers.
Do you have to be an AHCA NCAL member to register for IPCO?
No. Both AHCA NCAL members and nonmembers are eligible to participate in the IPCO course.
How much does it cost to take the IPCO training?
Registration fee: $450 AHCA NCAL members, $650 nonmembers. Payment and registration is completed by individual participant in the IPCO product in ahcancalED.
How can an individual register and pay for IPCO?
The individual who wants to take the IPCO course must login to ahcancalED and register for the course under their individual login which if you don’t have or forgot can easily set up by following the instructions. Payment will be made in ahcancalED upon registration via credit card or E-check. Please be sure to have your credit card or banking information ready at checkout. Paying by credit card or E-check will grant automatic access to the course. Registrations for IPCO cannot be done by another person or under another person’s ahcancalED login.
-- for a better web experience, please use Google Chrome Internet Browser and NOT Internet Explorer.
How can an organization group register and pay for IPCO?
Group purchase is available for groups of 5 or more. AHCA NCAL offers the following discount structure for groups: 5-49 registrations will receive $25 off each registration. 50 or more registrations will receive $75 off each registration.
After full payment is made for group purchase of IPCO, the designated individuals who the IPCO registration payment was made for, will be provided with a unique group code for their group which will translate to $0 due upon registration (because full payment has already been received). One code will be provided for each group with a max allowance of times that the code can be used based on the group’s payment.
Each individual will need to login to the AHCA NCAL website to access ahcancalED and then complete their own registration using the group code.
Can I get a refund on the IPCO product if I no longer want to take the course?
No refunds are issued for IPCO.
Can my IPCO registration be transferred to a colleague?
IPCO registrations cannot be transferred. The individual that registers for the course is the only one that has access to it.
Who is eligible to take this training?
Anyone can take this training. The AHCA NCAL Infection Preventionist Specialized Training does not require a particular healthcare license.
AHCA/NCAL recommends that administrators also consider taking the course to gain a deeper understanding of infection prevention and control in the overall operation of the building. Just a reminder that administrators should not serve as designated Infection Preventionists in Skilled Nursing Center per CMS regulations unless they have separate formal advanced clinical training and/or licensing such as a nursing license.
Please note, there are specific CMS requirements for the individual(s) who will serve as Infection Preventionist(s) in Skilled Nursing Center. While there are not currently any national requirements for assisted living facilities, states may establish specific requirements at some point.
CMS regulations for an person to serve as an IP in the Skilled Nursing Center is governed by 483.80 (b) Infection preventionist. The Skilled Nursing Facility must designate one or more individual(s) as the infection preventionist(s) (IPs) who are responsible for the facility’s IPCP. The IP must:
(1) Have primary professional training in nursing, medical technology, microbiology, epidemiology, or other related field;
(2) Be qualified by education, training, experience or certification;
(3) Work at least part-time at the facility; and
(4) Have completed specialized training in infection prevention and control.
What are the requirements to successfully complete IPCO?
Participate in each module and successfully complete quizzes throughout the course and final test (achieve at least 80% correct each time)
Modules 1-7 will have quizzes with 5 questions (4 of 5 questions must be accurately completed) except for module 3 which will have 10 questions (8 of 10 questions must be accurately completed).
The final test after Module 9 will have 125 questions (100 of 125 questions must be accurately completed).
Each module quiz may be attempted three times before the participant is required to repeat the module and then reattempt answering questions.
Complete course evaluation after each module and at the end of the course.
Course completion must occur within 12 months of the date the registrant starts the first required component of the program; which is the copyright agreement.(not registration date)
How long does it take on average to complete the IPCO course?
The learning time of all modules, review of additional resources, time to complete the modules and final course evaluations and quizzes/final test accounts for 25 hours and 30 minutes.
Participants are encouraged to spread out the course over time in an organized manner – such as scheduling module reviews on various dates/times when they can focus their attention to it. The course could be completed within a week or over several months based on how the individual would like to approach the program.
Are Contact Hours awarded for IPCO?
Yes, 25.5 ANCC contact hours and 28.75 hours continuing education hours (CEs) from the National Association of Long Term Care Administrator Boards (NAB) are available for completion of this program.
In support of improving patient care, this activity has been planned and implemented by University of Nebraska Medical Center and American Health Care Association. University of Nebraska Medical Center is jointly accredited by the Accreditation Council for Continuing Medical Education (ACCME), the Accreditation Council for Pharmacy Education (ACPE), and the American Nurses Credentialing Center (ANCC), to provide continuing education for the healthcare team.
What does a participant get when they complete the IPCO course?
Participants receive three certificates at the completion of IPCO:
- UNMC CON CiPDI will provide a certificate awarding 25.5 contact hours to participants who successfully achieve the completion requirements.
- 28.75 continuing education hours (CEs) from the National Association of Long Term Care Administrator Boards (NAB)
- Specialized Training Completion certificate from AHCA NCAL, valid for 3 years.
How long do the certificates last?
The CE certificates do not expire. The Specialized Training Completion certificate expires after 3 years from issue date.
How can someone renew their IPCO certificate?
Renewal may occur by the options below:
Option 1: Registering for a competency exam requiring a grade of 80% or above to successfully receive certificate of renewal. This option is only available to individuals who have previously successfully completed the full IPCO course and are seeking renewal.
Option 2: Registering for the IPCO course and completing the course requirements as outlined above.
Is IPCO a certification?
No, IPCO is a specialized training program with a certificate upon successful completion. While it is not a certification, IPCO does meet both the content and intensity/duration of CMS requirements to serve as an Infection Preventionist.
Does IPCO meet CMS requirements?
Yes, IPCO meets the expectations CMS has outlined on the required components of the specialized training.
CMS is not endorsing any particular training, rather CMS is focused on the content and intensity/duration of what will meet the specialized training requirement. Based on information AHCA NCAL received from CMS, the IPCO training meets both the content and intensity/duration of CMS requirements.
Can I print the presentation slides and how can I access the resources within the module?
Each module contains a resource guide which includes a copy of the presentation and any necessary supporting documents discussed within the module. This resource guide can be found at the top right corner within each module.
I am having technical difficulties with IPCO, can you help?
Please email us at educate@ahca.org.
How can an organization group register and pay for IPCO?
One user can purchase multiple registrations for other users by adding them to their cart during the checkout process; using the button displayed in image below. (This can only be done if all individuals have an ahcancalED account.) The price of the training will be based on each registrant’s member type (member or non-member).

*payment tip: please be sure when you are paying with a credit card the bill-to and shipping address are the same*
Group purchase is available for groups of 25 or more. If you are interested in group purchasing, please email educate@ahca.org
After full payment is made for group purchase, the designated individuals who the course registration payment was made for, will be provided with a unique group code for their group which will translate to $0 due upon registration (because full payment has already been received). One code will be provided for each group with a max allowance of times that the code can be used based on the group’s payment.
Each individual will need to login to the AHCA website to access ahcancalED and then complete their own registration using the group code.
PLEASE NOTE THAT WE ONLY ACCEPT PAYMENT IN THE FORM OF A CHECK FOR GROUP PURCHASES.
The NIPF is a national forum for any infection preventionist (IP) or infection prevention champions in long-term care (LTC) to share lessons learned and resources and get answers to questions.
This national forum will also provide a mechanism to rapidly disseminate federal updates and resources about infections in LTC as they become available from Centers for Disease Control and Prevention (CDC), Centers for Medicare and Medicaid Services (CMS), or Occupational Safety and Health Administration (OHSA). The American Health Care Association (AHCA) partnered with the Association for Professionals in Infection Control and Epidemiology (APIC) with funding from CDC Project First Line to set up the NIPF, which is open to all LTC professionals focusing on infection prevention regardless of their membership in AHCA or APIC.
The goal of NIPF is to foster collaboration and sharing of experiences between IPs in LTC. In addition, APIC and CDC subject matter experts will be available to address questions the group are unable to answer. There are designated threads for Hot Topics, Ask the CDC Expert, and test your clinical skills using Clinical Based Scenarios. The NIPF uses the “Connect Communities” platform to organize email discussions by threads and allows for sharing and posting of resources and tools in an organized library and ability to look up other IPs participating in the forum. You can receive email updates for threads in real-time or daily summaries.
To enroll in this national forum, all you need to do is fill out our form here https://www.ahcancal.org/Quality/Pages/NIPF and our team will process your application. If you have questions, please feel free to contact us at LTC-NIPFhelp@ahca.org.
-
Register
- Non-member - $650
- Member - $450
- *Further discounts may apply once you log in.
- More Information
- Added:
-
Contains 3 Component(s)
COVID-19 shed a spotlight on the need to improve infection prevention and control (IPC) programs in long term care. With emerging communicable diseases, including multidrug resistant organisms (MDROs), it is important for assisted living team members to understand standard, contact, and airborne precautions. This session reviews what an effective assisted living IPC program should include, the role quality improvement plays in assisted living IPC, the importance of understanding IPC precautions, and identifies the key stakeholders to engage in an IPC program.
Objectives: After attending this session, participants will be able to:
- Describe the significance of infections.
- Explain the chain of infection and how infection spreads.
- Discuss how to prevent the spread of infections.
- Identify elements to include in a written infection prevention and control program.
- Recognize themes and underlying causes of deficient infection prevention and control practices.
Speaker: Pamela Truscott, DNP/HSL, MSN/Ed, C-AL, DNS-CT, QCP, RAC-CT, CDP
Audience: All in assisted living
Length: 35 minutes
A certificate of completion is available (no CEs) upon successful completion
Cost:
$25 NCAL members
$65 Non-members
No CEs awarded upon completion.
Follow the Instructions Below to Register:
- To avoid technical problems, use Google Chrome.
- Members will need to log in using their existing email and password first.
- Once you are logged in to the website you will be able to register by clicking the green register button at the top of the page.
- If you have forgotten your password click here.
- If you are new to the site, you can create an account here. Answer all fields on the create an account page- especially locating your company name. You can search by name or zip code. After creating an account, you will be able to register.
Email educate@ahca.org if you need assistance.
Pamela Truscott, DNP/HSL, MSN/Ed, RN, DNS-CT, QCP, RAC-CT, CDP (Moderator)
Director of Quality Improvement
NCAL
Pamela Truscott, DNP/HSL, MSN/Ed, RN, DNS-CT, QCP is the Director of Quality Improvement with the National Center for Assisted Living (NCAL). She joined the AHCA/NCAL family in June 2019 and has been actively involved with a variety of education, tools and resources such as: trauma-informed care, behavioral health, functional outcomes improvement, and infection prevention and control. Prior to joining AHCA, Pam worked for the Nebraska Health Care Association (NHCA) as the Vice President of Professional Development for seven years and is a Nebraska Assisted LIving Administrator. Before joining the NHCA team, she worked in a rural nursing home with attached assisted living community for 15 years in a variety of roles, including: charge nurse, wound nurse, medication aide, and direct care staff member. She is an active member in the American Nurses Association as well as the American Association of Post-Acute Care Nurses. She received a Doctor of Nursing Practice with specialy focus in Healthcare Systems Leadership and Master of Science in Nursing with focus in nursing education degree from Chamberlain College of Nursing. Pam has over 20 years of long-term care experience and shares a passion for growing education and cultivating new leaders in long-term care.
-
Register
- Non-member - $65
- Member - $25
- *Further discounts may apply once you log in.
- More Information
-
Contains 18 Component(s), Includes Credits
Component Credit Type State/Medical Type Available Credits Earned Credits Certificate of Completion - 20230704-3.50-A86038-DL Medical NAB 3.50 0.00 Working in post acute and long term care is incredibly rewarding. It is also stressful due to the demands and pressures that are faced on a daily basis. The workforce crisis and COVID-19 have exacerbated this stress creating even more challenges for those who work in long term care. This course is aimed at reinvigorating your passion for long term care by providing you with tools and resources you can immediately use to decrease your perceived stress levels and help your team members do the same to aid with staff retention. Self-care is essential and is the key to self-managing stressful situations. If you are not taking care of yourself first, how can you be expected to take care of others? It is time to put yourself first! Mindfulness-based stress reduction learned in this training can help put self-care back into your daily routine and support you in doing what you do best.
Course Objectives:
- Identify what stress is.
- Identify why we fail at self-care.
- Examine the importance of self-care.
- Describe the mindfulness-based stress reduction (MBSR) program.
- Discuss how to use the MBSR program to improve staff retention, resiliency, and improve job satisfaction.
- Describe how to establish a MBSR program peer support group.
- Discuss the sustainability of MBSR programs.
- Identify which MBSR program strategy you can implement today to decrease your stress.
Presenter: Pamela Truscott, MSN/Ed, DNS-CT, QCP, RAC-CT, CDP, Director, Clinical and Regulatory Services
Cost:
$99 for AHCA/NCAL members
$149 for non-members
Additional discounts are available for groups 26+
3.50 NAB CEs and 3.0 contact hours are available upon course completion.
© 2022 American Health Care Association. All rights reserved.
All Improving Staff Resiliency and Retention: An Action Plan that Works materials subject to this copyright may be photocopied or distributed for the purpose of nonprofit or educational advancement. The use, photocopying, and distribution for commercial purposes of any of these materials is expressly prohibited without the prior written permission of American Health Care Association.
Please use Google Chrome for the best user experience.
One individual can purchase multiple registrations for more participants by adding them to their cart during the checkout process. Please note, for this option to work, every participant will need to have an ahcancalED account first.
To add several participants, please click the green button in the cart that says:
 .
.
You will then be able to search for more than one participant using their email address. If the person making payment should not have access to the course, then you can remove yourself by clicking the red "remove" button by your name.
*Payment Tip: The price of the training will be based on each registrant’s member type (member or non-member). please be sure when you are paying with a credit card the bill-to and shipping address are the same*
If you need assistance, please email educate@ahca.org

Compassion Fatigue and Burnout in Nursing, Second Edition
Savings: SAVE 30%: enter code AHCANCAL30 at check out.-
Register
- Non-member - $149
- Member - $99
- *Further discounts may apply once you log in.
- More Information
-
Contains 3 Component(s)
Long term care facilities are incredibly stressful environments. Working with people can be stressful. The staffing crisis and COVID-19 have exacerbated the stress creating even more challenges for those who work in long term care. This session is aimed at reinvigorating your passion for long term care by providing you with tools and resources you can immediately use to decrease your perceived stress levels and help your team members do the same. Self-care is absolutely essential and is the secret to surviving stressful situations. If you are not taking care of yourself first, how can you be expected to take care of others. It is time to put yourself first!
Learning Objectives:
- After attending this session, participants will be able to:
- Identify stressful situations within their environment.
- Employ stress reduction techniques that work.
- Decrease their overall perceived stress levels.
Presenter:
Pamela Truscott MSN/Ed, DNS-CT, QCP, RAC-CT, CDP
Cost:
$25 AHCA/NCAL Members
$65 Non-members
This 34-minute learning session does not come with CEs.
© 2022 American Health Care Association. All rights reserved.
All Self-Care: The Secret to Surviving! materials subject to this copyright may be photocopied or distributed for the purpose of nonprofit or educational advancement. The use, photocopying, and distribution for commercial purposes of any of these materials is expressly prohibited without the prior written permission of American Health Care Association.
Please use Google Chrome for the best user experience.
One individual can purchase multiple registrations for more participants by adding them to their cart during the checkout process. Please note, for this option to work, every participant will need to have an ahcancalED account first.
To add several participants, please click the green button in the cart that says:
 .
.
You will then be able to search for more than one participant using their email address. If the person making payment should not have access to the course, then you can remove yourself by clicking the red "remove" button by your name.

*Payment Tip: The price of the training will be based on each registrant’s member type (member or non-member). please be sure when you are paying with a credit card the bill-to and shipping address are the same*
If you need assistance, please email educate@ahca.org

Compassion Fatigue and Burnout in Nursing, Second Edition
Savings: SAVE 30%: enter code AHCANCAL30 at check out.-
Register
- Non-member - $65
- Member - $25
- *Further discounts may apply once you log in.
- More Information
- After attending this session, participants will be able to:
| Access Date | Quiz Result | Score | Actions |
|---|
Welcome
Log in using your ahcancal username and password.

